Eczema is a common skin condition that causes dry, itchy, and inflamed skin. It can affect people of all ages, though it is particularly common in children. The appearance and cause of eczema can vary, so it is often classified into different types.
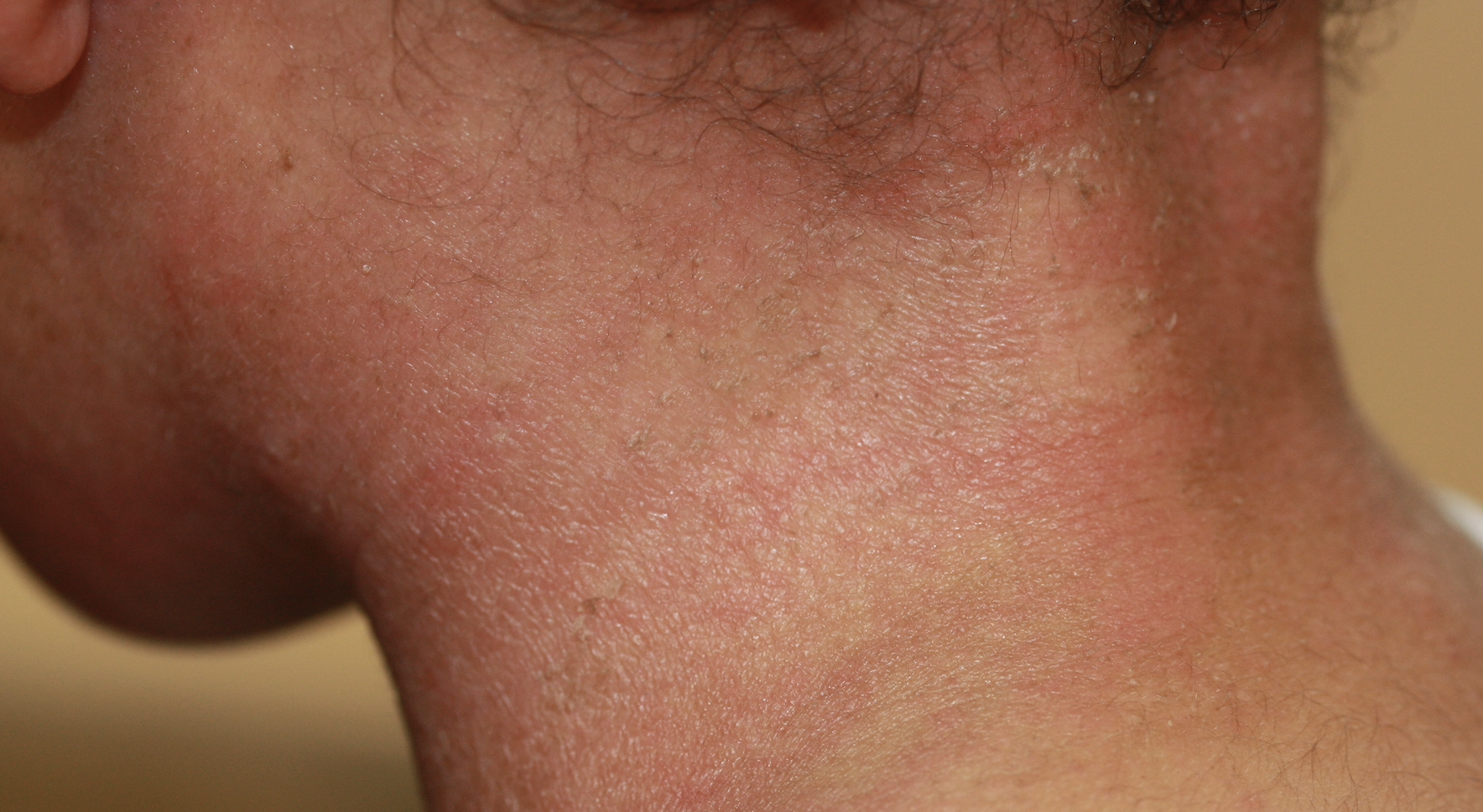
The most common form, usually beginning in infancy or childhood. It often occurs in children with a family history of asthma, eczema, or hay fever (atopy).
Similar in appearance to atopic eczema but without a background of allergies or hay fever.
Round, coin-shaped patches that typically appear on the arms and legs.
Dry, itchy inflammation on the lower legs, often in older adults and linked to varicose veins or leg swelling.
Caused by an allergic reaction to something touching the skin, such as nickel, fragrance, or certain chemicals.
Triggered by frequent contact with substances that dry out or irritate the skin, such as detergents or cleaning products.
Sometimes, more than one factor contributes to eczema, and the pattern may not fit neatly into one category.
Eczema itself is not caused by an allergy, but in some children with severe or difficult-to-control eczema, food allergies may contribute to flare-ups.
If a child has a consistent or immediate reaction to a particular food, especially alongside symptoms such as tummy pain, vomiting, diarrhoea, constipation, lip or facial swelling, or poor growth, allergy testing may be considered. Your consultant dermatologist will discuss whether this is appropriate.
Contact dermatitis, however, is caused by an allergic reaction to substances in the environment, and it can be relevant in cases of hand or face eczema. It is particularly common in certain occupations such as hairdressing, catering, or floristry. Patch testing may be used to identify the cause.
Eczema is mainly a problem of dry and inflamed skin. There is no single cure, but simple and consistent treatment can keep it under control and significantly improve symptoms.
These are moisturising treatments that help repair the skin barrier and reduce dryness. They should be used generously and regularly:
Bath oils or emollient washes help clean and hydrate the skin.
They gently cleanse the skin while locking in moisture.
Apply liberally at least twice daily, ideally more often.
Your dermatologist will recommend suitable products, as there are many different formulations.
Topical corticosteroids are the first-line treatment for eczema (as recommended by NICE). They reduce inflammation and itching.
It is more effective to use a steroid strong enough to settle the eczema quickly and then switch to intermittent maintenance use, rather than using a weak steroid for long periods with poor results.
Skin thinning is a common concern, but when steroids are prescribed appropriately and supervised by your dermatologist, this risk is minimal. Potent steroids are rarely used in children and only for short, targeted courses.
Medications such as tacrolimus (Protopic) and pimecrolimus (Elidel) are second-line treatments for eczema that has not responded to topical steroids, or where steroid side effects are an issue.
They are particularly useful on delicate areas such as the face. Different strengths are available for different ages, and your dermatologist will explain how and when to apply them.
Can help reduce itching during the day.
Can be useful at night to improve sleep when itching is severe.
These are specialised dressings taught by dermatology nurses to soothe and protect the skin.
Occasionally considered for children with proven food allergies, but only under medical and dietetic supervision to avoid nutritional deficiencies.
In severe or resistant cases, treatments such as oral steroids, methotrexate, or ciclosporin may be prescribed by a consultant dermatologist or paediatrician.
May benefit from additional treatments such as compression bandaging, which your consultant will discuss if appropriate.
Children with atopic (allergy-type) eczema often improve as they grow, with most outgrowing the condition by school age. A small number may experience occasional flare-ups during adolescence, and some continue to have symptoms into adulthood.
Other forms, such as contact dermatitis, usually improve once the trigger has been identified and avoided. With good skincare and appropriate medical guidance, long-term control is achievable for most people.