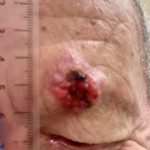
 The three common skin cancers are basal cell carcinomata (BCC), squamous cell carcinomata (SCC) and malignant melanomas (MM). In the UK on the NHS, these skin cancers are triaged into their respective urgencies in order to best utilise health care resources. So basal cell carcinomata are triaged as routine referrals because they are slow growing and by and large, do not metastasise or spread around the body. However, SCCs and MMs do have the potential to spread and hence are triaged as urgent. Any lesion suspected of being either of these should be referred to dermatology as a 2-week wait, ie is seen within 2 weeks of referral and many are removed at the appointment or within the next couple of weeks.
The three common skin cancers are basal cell carcinomata (BCC), squamous cell carcinomata (SCC) and malignant melanomas (MM). In the UK on the NHS, these skin cancers are triaged into their respective urgencies in order to best utilise health care resources. So basal cell carcinomata are triaged as routine referrals because they are slow growing and by and large, do not metastasise or spread around the body. However, SCCs and MMs do have the potential to spread and hence are triaged as urgent. Any lesion suspected of being either of these should be referred to dermatology as a 2-week wait, ie is seen within 2 weeks of referral and many are removed at the appointment or within the next couple of weeks.
If they are confirmed to be an SCC or an MM, then all cases are discussed at a skin multidisciplinary meeting or MDM to decide the best plan of management. At these meetings there are dermatologists, plastic surgeons, oncologists, radiologists, skin cancer specialist nurses, MDM co-ordinators and administrative staff. If you are a doctor involved in skin cancer management, attendance at these MDMs is necessary.
For melanomas, the current plan of management is fairly straightforward. All MMs go on to have a further wider excision of the scar and patients with MMs above a certain thickness or activity will be offered something called a sentinel lymph node biopsy. Certain thick or highly active MMs will require regular PET-CT imaging. Mutation analysis will be performed on the samples. All patients with MMs will have follow up, the length of which depends on the thickness of the MM.
However for SCCs, as long as the SCC is removed with a good margin of normal skin, most patients just have a few regular skin checks and lymph node checks for a period of time ranging up to around 2 years. Certain patients with head and neck SCCs may be offered an ultrasound scan of their neck lymph nodes. And that’s it!
So if an SCC is going to metastasise, we simply have to wait for it to metastasise before anything is done.
It was therefore interesting to read about a study looking at protein expressions in SCCs in the April 2021 edition of the British Journal of Dermatology.
[Shapanis A, Lai C, Smith S et al. Identification of proteins associated with development of metastasis from cutaneous squamous cell carcinomas (cSCCs) via proteomic analysis of primary cSCCs. Br J Dermatol 2021;184:709-721.]
What did this look at?
They looked at 105 completely excised primary cSCCs. 52 of these had metastasised and 53 had not metastasised at 5 years post surgery. Surprisingly, this has not been looked at before.
What did they find?
They found 33 significantly differentially expressed proteins between the cSCCs that metastasised and those that had not.
More specifically, they found that raised levels of two specific proteins were associated with a reduced time to metastasis from the primary cSCC.
What were these two proteins called?
They were called ANXA5 and DDOST. Their long names are annexin A5 and (wait for it!) dolichyl-diphosphooligosaccharide-protein glycosyl-transferase noncatalytic subunit (you need to have your Weetabix to deal with that daily…)
And were the results reliable?
They showed that these two proteins had an accuracy of 92.1% and also a higher sensitivity and specificity than current cSCC staging systems in clinical use.
So can we start using them now?
Well no.
Both proteins have been looked at to some degree in the past. ANXA5 has previously been shown to be an unfavourable prognostic marker in kidney, liver, urinary tract, head and neck cancers but a favourable marker in womb and stomach cancers.
There is much more limited research on DDOST (with that name, what do you expect?) but it also has been found to be an unfavourable prognostic marker in kidney, liver, and head and neck cancers but a favourable marker in womb cancer.
So in the future?
This was a fairly small study and much larger, so called cohort studies need to be performed. I think their use will not be on their own as stand alone prognostic markers but their incorporation with other clinical and pathological markers will give rise to a better prediction model as to which SCCs will metastasise or not.
Kind regards,
Sandy
Dr Sandy Flann, Consultant Dermatologist
