 There have been recent major advances in the understanding of what causes eczema and it all concerns a molecule called filaggrin.
There have been recent major advances in the understanding of what causes eczema and it all concerns a molecule called filaggrin.
[Brown SJ and McLean WHI. One remarkable molecule: Filaggrin. J Invest Dermatol 2012; 132(3 Pt 2): 751-762.]
Now, there is a common dry skin disorder called ichthyosis vulgaris. It is an inherited skin condition but its severity, and therefore clinical appearance can vary greatly within an affected family so that some family members may be unaware that they have the condition. By and large, it causes no problems but if you were to experience anything it would usually be fine scaling on the outer parts of the legs and arms or on the lower tummy which is typically worsened with cold, dry weather and can even resolve completely in a hot, humid environment.
Affected individuals may also suffer from another skin condition called keratosis pilaris. This is another common, inherited skin condition which typically affects the outer parts of the arms and legs but could also be present on the cheeks or tummy. One would expect to see rough spots which can be reddish in these areas.
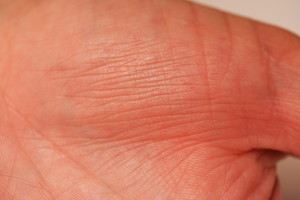
Another feature of ichthyosis vulgaris is on the palms. These are not scaly but what we call, hyperlinear, ie have extra lines, especially on the area around the base of the thumb (what we call the thenar eminence).
So what does this all have to do with filaggrin?
In 2006, it was discovered that mutations in the gene for the protein filaggrin were the cause of ichthyosis vulgaris.
[Smith FJ, Irvine AD, Terron-Kwiatkowski A et al. Loss-of-function mutations in the gene encoding filaggrin cause ichthyosis vulgaris. Nat Genet 2006; 38: 337-342.]
Filaggrin is a protein which helps knit the skin barrier together, preventing water loss from the skin and also reducing the ability of allergens and micro-organisms to enter through the skin.
Filaggrin, when broken down on the skin surface, also goes on to produce so-called ‘natural moisturizing factor’ which also helps to keep the skin hydrated and act as a barrier. Filaggrin breakdown products also inhibit the growth of micro-organisms such as Staphylococcus aureus, a common organism found on the skin of eczema patients.
Ok, but what evidence is there linking filaggrin and eczema?
As ichthyosis vulgaris and eczema are commonly found together, it was logical therefore to investigate whether filaggrin was involved in the development of eczema. There have now been 20 or more studies confirming a strong and highly significant association between mutations in the filaggrin gene and atopic eczema, especially early onset, severe or persistent eczema.
[Brown SJ, Sandilands A, Zhao Y, et al. Prevalent and low-frequency null mutations in the filaggrin gene are associated with early-onset and persistent atopic eczema. J Invest Dermatol 2008; 128: 1591-1594.]
In addition, filaggrin mutations have also been found to be a risk factor in something called the ‘atopic march’.
What is the ‘atopic march’?
This is where atopic eczema is found to precede the development of food allergies, hayfever and asthma in chronological order.
[Brown SJ, Relton CL, Liao H, et al. Filaggrin null mutations and childhood atopic eczema: a population-based case-control study. J Allergy Clin Immunol. 2008; 121: 940-946.]
[Brown SJ, Asai Y, Cordell HJ, et al. Loss-of-function variants in the filaggrin gene are a significant risk factor for peanut allergy. J Allergy Clin Immunol. 2011; 127: 661-667.]
[Schuttelaar ML, Kerkhof M, Jonkman MF, et al. Filaggrin mutations in the onset of eczema, sensitization, asthma, hay fever and the interaction with cat exposure. Allergy. 2009; 64: 1758-1765.]
A recent large study looked at the role of filaggrin mutations, development of eczema and development of sensitization to allergens such as food allergens and airborne allergens (eg cat and dog dander, pollens). It involved 1,456 children born on the Isle of Wight, UK in 1989 and the study followed them up until the children were aged 18-years.
It found that if a child had a filaggrin mutation this increased their chances of developing eczema two-fold but if that child then became sensitized to an allergen, this combined effect led to an even stronger risk that that child would develop eczema. This applied particularly to early childhood (ages 1-4years) but also covered the first two decades of life.
[Ziyab AH, Karmaus W, Yousefi M, et al. Interplay of filaggrin loss-of-function variants, allergic sensitization, and eczema in a longitudinal study covering infancy to 18 years of age. PLoS ONE 2012; 7(3): e32721.]
What does this mean to me, especially if I have a young child with eczema?
There is, therefore clear evidence that treating eczema aggressively in early childhood and thereby improving skin barrier function may help to prevent sensitization to environmental allergens and possibly also development of food allergies, hayfever and asthma in later life.
Regards,
Sandy
Dr Sandy Flann, Consultant Dermatologist
