 The vast majority of our workload at the Dermatology department at Orpington Hospital deals with skin cancer and by far and away the commonest skin cancer we deal with is called a basal cell carcinoma (BCC). Its other name is ‘rodent ulcer.’ Indeed in my adult general clinic today nearly all my patients had a BCC and our theatre lists do get quite booked up with removing them all!
The vast majority of our workload at the Dermatology department at Orpington Hospital deals with skin cancer and by far and away the commonest skin cancer we deal with is called a basal cell carcinoma (BCC). Its other name is ‘rodent ulcer.’ Indeed in my adult general clinic today nearly all my patients had a BCC and our theatre lists do get quite booked up with removing them all!
Where on the body do you get BCCs?
BCCs commonly occur on sun-exposed sites of fair skinned individuals who have had a lot of sun exposure over many years. However, sun exposure is not the whole story as BCCs can be found in sites on the body which are sheltered from the sun and there are also some genetically inherited conditions which hugely increase your risk of developing BCCs.
How do I know if I have a BCC?
The typical history of a patient presenting with a BCC is of a pink or flesh-coloured spot that either doesn’t bother them or itches slightly. Many patients describe them as ‘irritating’ or ‘an irritation.’ The majority of patients have had their lesion for some time; anything from 6 months to more than 2 years at presentation to us. The ‘irritation’ tends to break down, ulcerate, scab up but always fails to heal up completely or go away.
What does a BCC look like?
When you look closely at a BCC under a good light, a BCC has several classical features. Dermatologists look for a shiny appearance with little vessels coursing over the surface which we call ‘arborising telangiectasiae.’ The edge of a BCC is described as looking rolled and pearly and this is the typical description of a nodular or nodulocystic BCC.
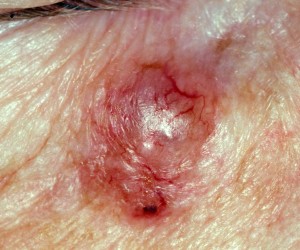
There are, however, other forms of BCC. Some can look like flat, red scaly patches, some can look like whitish scars and some can look dark.


And of course there is the rodent ulcer form where the skin has broken down in the area to form an ulcer in the centre.
Because they are painless, cause only minimal problems and are slow growing, they are easy to overlook and we have had, not too uncommonly, an elderly patient presenting with a quite large BCC which they have put off seeing their doctor about.
How do you treat a BCC?
The treatment is, in the main, surgical and if the BCC is removed properly it shouldn’t come back. It has been shown that to ensure complete removal and reduce the risk of recurrence, a pre-determined area of normal skin around the BCC is also removed at the time as the BCC. This can mean that quite a large area of skin is removed for what seems like a small, innocuous pink spot. Therefore, if a BCC is allowed to grow to quite a size, the removal can be quite difficult.
Who should I see to remove a BCC?
BCCs in areas prone to recurrence such as the head and neck should be seen by a dermatologist in the first instance according to NICE guidance [see http://www.nice.org.uk/nicemedia/live/10901/48878/48878.pdf NICE guidance on Cancer Services: Improving Outcomes for People with Skin Tumours including Melanoma (update)].
Many small BCCs on the head and neck can, and are removed routinely by dermatologists. In some cases, especially if they are quite large or in an area of the face where it is important to preserve the skin and its contours eg around the eye, nose or mouth, patients may be referred to a plastic surgeon, a maxillofacial surgeon or a dermatological surgeon (who may perform Moh’s micrographic surgery – a very specialized form of skin surgery).
Not every patient who has had a single BCC needs regular dermatological review however I do see patients regularly who have had several BCCs as their likelihood of developing another BCC (or a squamous cell carcinoma or a melanoma, for that matter) is quite high.
Sandy
Dr Sandy Flann, Consultant Dermatologist
