A common, minor form of skin cancer
Basal Cell Carcinoma (Rodent Ulcer or BCC) Explained
What is a basal cell carcinoma?
A basal cell carcinoma (BCC) is a common and usually minor form of skin cancer. It develops from the basal cells, which sit at the bottom of the outer layer of the skin (the epidermis).
BCCs grow slowly and rarely spread to other parts of the body. However, if left untreated, they continue to grow and can extend into the deeper layers of the skin and surrounding tissue. Over time, this can cause local damage, particularly if the lesion is close to the eyes, nose, or ears.
Larger, untreated BCCs may ulcerate (break down into sores), bleed, or become infected. Early diagnosis and treatment offer an excellent outcome and help prevent more complicated surgery later.
What causes BCCs?
Most BCCs are linked to sun exposure, either from regular sun exposure over many years or from episodes of sunburn, particularly in childhood.
They are most often found on areas of the body that receive the most sunlight, such as the face and neck, the upper back (particularly in men), and the lower legs (more common in women).
People most at risk include those who:
Have fair skin that burns easily.
Have spent long periods abroad or outdoors without adequate sun protection.
Work outside or enjoy outdoor hobbies such as gardening, sailing, or golf.
Using sunscreen, covering up, and avoiding deliberate tanning all help reduce the risk.
What does a BCC look like?
There are several different forms of BCC, and their appearance can vary:
Superficial BCC:
Flat, red, scaly patches that may resemble eczema or psoriasis.
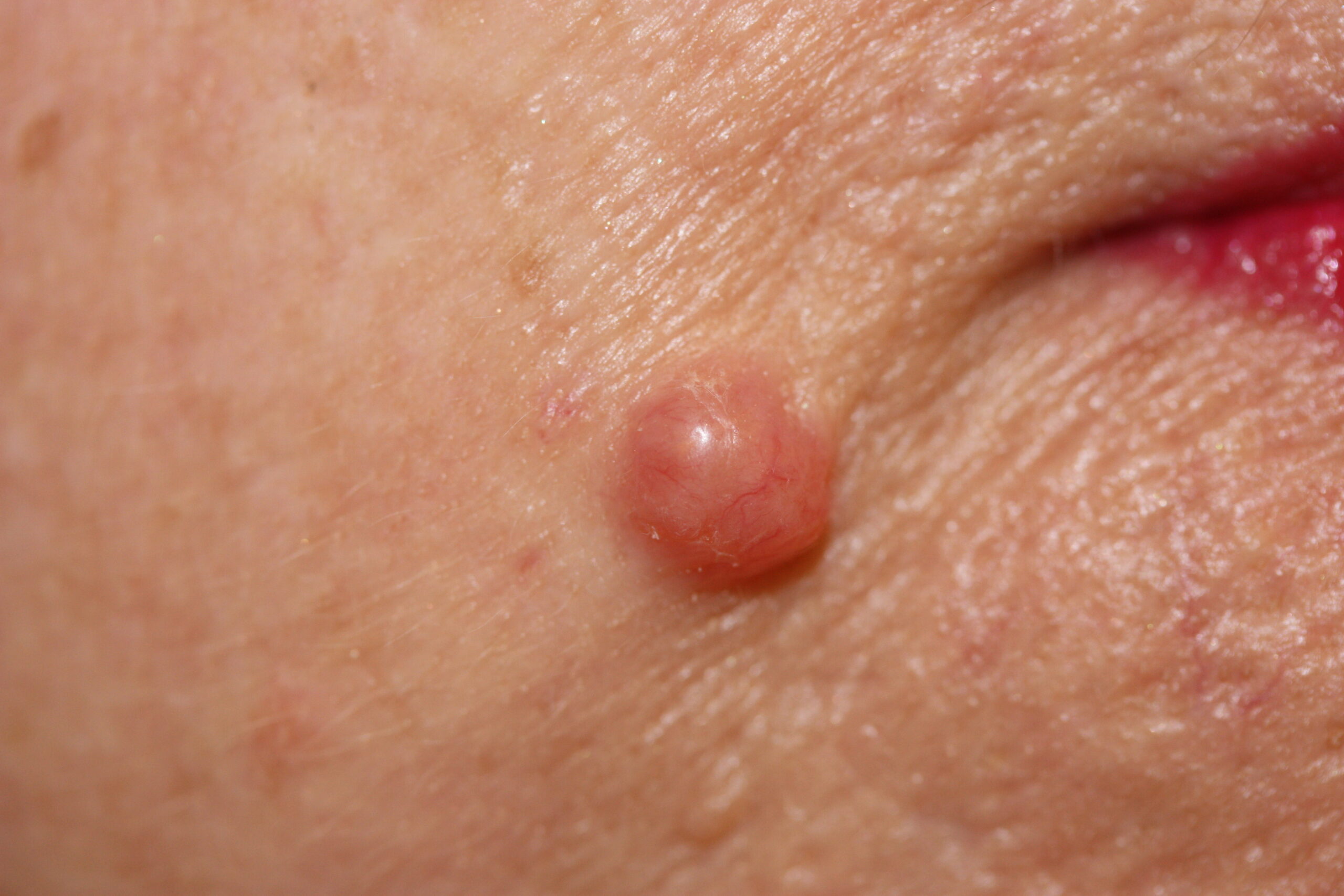
Nodular BCC
Shiny, pale pink or red nodules that can appear pearly or translucent.
Morphoeic BCC
Scar-like, waxy patches that may look slightly sunken or pale.
Ulcerated BCC (rodent ulcer)
An open sore that repeatedly scabs, bleeds, and fails to heal.
Any new, persistent, or changing patch or lump on the skin should be assessed by a dermatologist.
How are BCCs treated?
Treatment depends on the size, type, and location of the BCC. Dr Flann offers a full range of evidence-based options:
Topical treatments (creams):
Medications such as 5-fluorouracil or imiquimod may be used for small, superficial BCCs confirmed by biopsy. These can cause redness and soreness during treatment, which is expected.
Surgical treatments:
- Curettage and cautery: The BCC is gently scraped away under local anaesthetic, and the base is cauterised (burnt) to destroy any remaining cancer cells.
- Excision: The BCC is surgically removed, and the wound is repaired with stitches.
- Plastic surgery reconstruction: Larger lesions or those in delicate areas may require a skin flap or graft to achieve the best cosmetic result.
- Mohs micrographic surgery: A specialist technique performed in select centres. The tumour is removed in stages, and each layer is examined under a microscope immediately. The process is repeated until no cancer cells remain. This method is especially useful for facial BCCs or those with unclear edges.
Radiotherapy
Used when surgery is not suitable. It involves multiple treatment sessions over several weeks and is highly effective for certain cases.
Vismodegib
A targeted medication reserved for very advanced BCCs that cannot be treated surgically. It is prescribed only in tertiary referral centres.
What happens after treatment?
Once a BCC has been successfully treated, the outlook is excellent. Most cases are completely cured and do not recur.
However, because people who have had one BCC are at increased risk of developing another, it is important to:
Check your skin regularly for new growths or sores that do not heal.
Protect your skin from the sun year-round using sunscreen (SPF 30+), protective clothing, and shade.
Attend follow-up appointments if advised by your consultant dermatologist.
Regular self-checks and prompt assessment of any suspicious area help ensure early treatment and the best possible outcome.